 Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or
Read more
Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or
Read more



My Blog
-
Mole Check: Importance of Regular Skin Exams for Early Detection
posted: Apr. 02, 2024.
 Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or
Read more
Moles are common skin growths that can appear anywhere on the body. While most moles are harmless, changes in size, shape, color, or texture can sometimes indicate skin cancer or
Read more
-
What You Need To Know About Cosmetic Dermatology
posted: Mar. 01, 2024.
 Cosmetic dermatology is focused on you looking your best. No matter what the aesthetic concern is, there is a procedure to help minimize the problem, so you can look great.
Read more
Cosmetic dermatology is focused on you looking your best. No matter what the aesthetic concern is, there is a procedure to help minimize the problem, so you can look great.
Read more
-
Cosmetic Dermatology: Exploring Non-Surgical Aesthetic Procedures
posted: Feb. 01, 2024.
 Cosmetic dermatology focuses on enhancing the appearance of the skin, offering treatments aimed at refining, rejuvenating, and correcting various skin concerns. Cosmetic dermatology doesn't revolve around vanity. It boosts confidence
Read more
Cosmetic dermatology focuses on enhancing the appearance of the skin, offering treatments aimed at refining, rejuvenating, and correcting various skin concerns. Cosmetic dermatology doesn't revolve around vanity. It boosts confidence
Read more
-
Common Skin Conditions
posted: Jan. 01, 2024.
 A dermatologist is a specialized medical professional focused on skin health. They're like skin detectives, trained extensively to diagnose, treat, and manage various skin, hair, and nail conditions. From acne
Read more
A dermatologist is a specialized medical professional focused on skin health. They're like skin detectives, trained extensively to diagnose, treat, and manage various skin, hair, and nail conditions. From acne
Read more
-
Managing Chronic Skin Conditions
posted: Dec. 01, 2023.
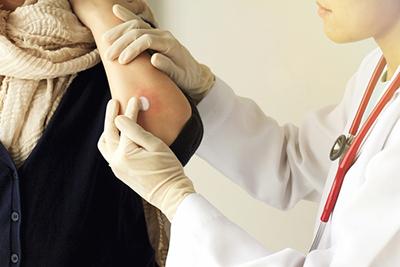 Chronic skin conditions can be embarrassing and uncomfortable. You may be able to manage a minor chronic skin condition on your own. For other chronic skin conditions, you can benefit
Read more
Chronic skin conditions can be embarrassing and uncomfortable. You may be able to manage a minor chronic skin condition on your own. For other chronic skin conditions, you can benefit
Read more
-
Rosacea: Understanding Triggers and Effective Treatment Approaches
posted: Nov. 01, 2023.
 Rosacea is a chronic skin condition causing redness, visible blood vessels, and sometimes bumps on your face. Its exact cause isn't clear, but triggers like sunlight, stress, spicy food, and
Read more
Rosacea is a chronic skin condition causing redness, visible blood vessels, and sometimes bumps on your face. Its exact cause isn't clear, but triggers like sunlight, stress, spicy food, and
Read more
-
What Can a Chemical Peel Do for Your Skin?
posted: Oct. 01, 2023.
 A chemical peel is a cosmetic procedure in which a dermatologist applies a chemical solution to the skin to remove damaged outer layers, revealing smoother, more youthful-looking skin. Chemical peels
Read more
A chemical peel is a cosmetic procedure in which a dermatologist applies a chemical solution to the skin to remove damaged outer layers, revealing smoother, more youthful-looking skin. Chemical peels
Read more
-
Why Taking Care of Your Skin Is Important
posted: Sep. 01, 2023.
 Your skin performs many important functions including protecting your vulnerable internal organs, protecting you from bacteria and viruses, and helping you look your best. Taking care of your skin is
Read more
Your skin performs many important functions including protecting your vulnerable internal organs, protecting you from bacteria and viruses, and helping you look your best. Taking care of your skin is
Read more
-
The Power of Chemical Peels
posted: Aug. 01, 2023.
 When you have healthy skin, with an even skin tone, you just naturally look better. You look younger and more vibrant. Unfortunately, aging, sun exposure, environmental toxins, and other factors
Read more
When you have healthy skin, with an even skin tone, you just naturally look better. You look younger and more vibrant. Unfortunately, aging, sun exposure, environmental toxins, and other factors
Read more
-
Treating Eczema in Adults
posted: Jul. 01, 2023.
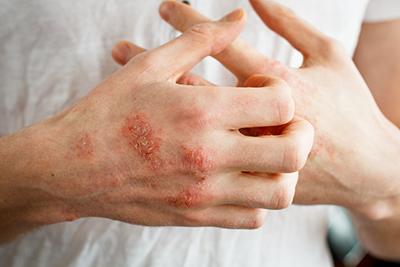 Eczema, also known as atopic dermatitis, is a chronic skin condition characterized by red, itchy, and inflamed patches on the skin. It affects millions of people worldwide, both children and
Read more
Eczema, also known as atopic dermatitis, is a chronic skin condition characterized by red, itchy, and inflamed patches on the skin. It affects millions of people worldwide, both children and
Read more
-
Treatment Options for Acne Scarring
posted: Jun. 05, 2023.
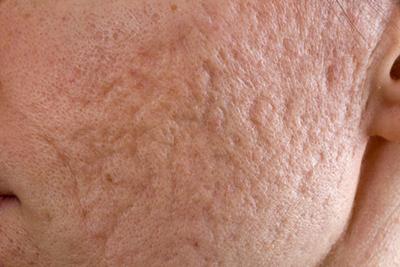 Acne is a common problem, and it’s a problem that may continue with acne scarring. If you have acne scarring, you will be happy to know that your dermatologist can
Read more
Acne is a common problem, and it’s a problem that may continue with acne scarring. If you have acne scarring, you will be happy to know that your dermatologist can
Read more
-
Eczema: Understanding Triggers and Treatment Options
posted: May 02, 2023.
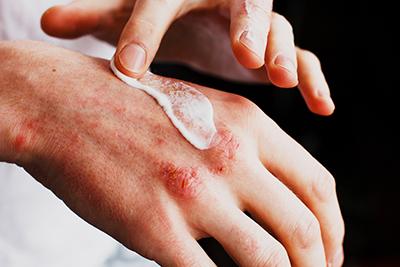 Eczema is a skin condition that can leave you feeling itchy and dry. Dealing with eczema can be annoying and you might find that a flare-up can be irritating and
Read more
Eczema is a skin condition that can leave you feeling itchy and dry. Dealing with eczema can be annoying and you might find that a flare-up can be irritating and
Read more
-
Skin Cancer Prevention Tips
posted: Apr. 05, 2023.
 It feels great to be out in the sun. Unfortunately, while you are enjoying yourself, the sun is damaging your skin. Excessive sun exposure can lead to skin cancer. There
Read more
It feels great to be out in the sun. Unfortunately, while you are enjoying yourself, the sun is damaging your skin. Excessive sun exposure can lead to skin cancer. There
Read more
-
Understanding Common Skin Conditions and How to Manage Them
posted: Mar. 09, 2023.
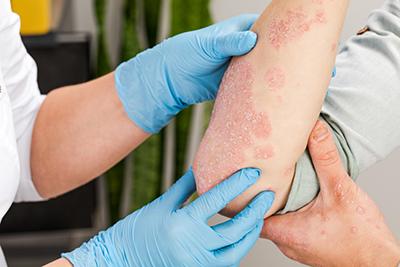 There are many skin disorders that people struggle with, and they vary greatly in symptoms and their severities. Some skin conditions can be temporary, while others are permanent and have
Read more
There are many skin disorders that people struggle with, and they vary greatly in symptoms and their severities. Some skin conditions can be temporary, while others are permanent and have
Read more
-
How to Treat and Prevent Eczema Flare-Ups
posted: Feb. 06, 2023.
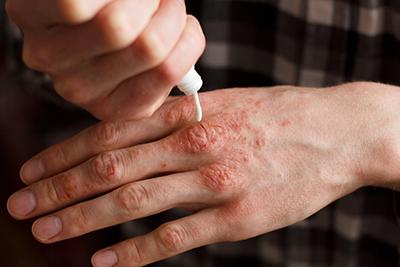 If you deal with eczema, you understand that dealing with a flare-up can be irritating and can distract from your normal routine. You might also feel self-conscious about it being
Read more
If you deal with eczema, you understand that dealing with a flare-up can be irritating and can distract from your normal routine. You might also feel self-conscious about it being
Read more
This website includes materials that are protected by copyright, or other proprietary rights. Transmission or reproduction of protected items beyond that allowed by fair use, as defined in the copyright laws, requires the written permission of the copyright owners.
